Treatment Delivery
Can we please get your advice on this one question?
- Patient Position
- Isocenter
- Treatment Parameters
- Prescription
- Modality
- Auxiliary Set-Up Devices
- Machine Operation
- Beam Modifiers
- Patient Monitoring Systems
- Record and verify Systems
- Portal Imaging
- Site Verification
- Dose Verification
- Equipment Malfunctions
- Documentation
- Information in Treatment Record
- Elements of record Keeping
- Charge Capture Terminology
Verification > Patient Position
Verification > Isocenter
Verification >Treatment Parameters
Verification > Prescription
Verification > Modality
Treatment Machine Set-Up > Auxiliary Set-Up Devices
Treatment Machine Set-Up > Machine Operation
- Console controls
Machine
operation is the significant role in all the fields. In radiotherapy also it’s important because
here small mistakes make big impact in the treatment. However, a few errors are always there in
machine operation like setup, digital indication errors etc. In order to rule out those errors advance
technology machines are introduced and some are in research process.
Machine operation Radiotherapy:
Machine operation in radiotherapy is different for different machines.
Operations in Teletherapy,
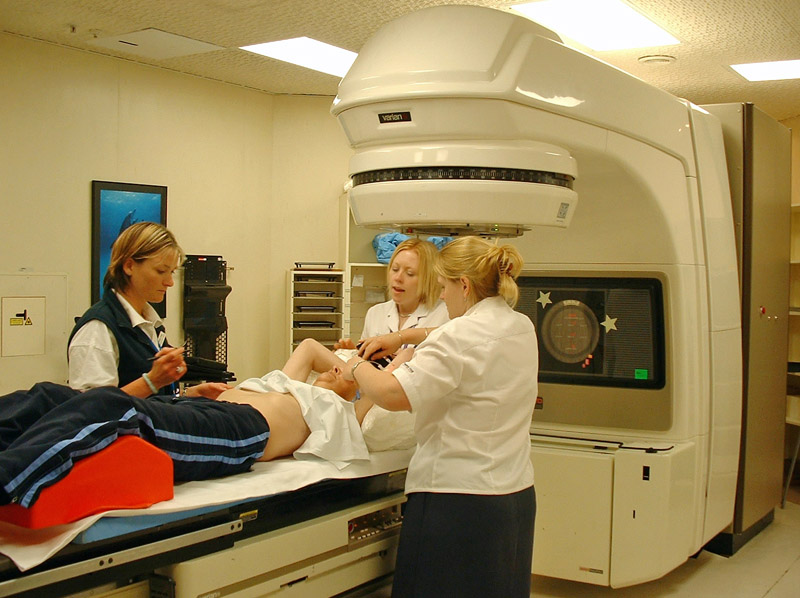
- Patient positing is one of the major were the errors occur. These errors indirectly related to the machine operation. If, radiation therapist doesn’t operate the machine of set the patient in exact position means errors will come, inevitably leads incorrect treatment.
- In teletherapy machines such as Cobalt-60 based or Linear Accelerators are fully computerized to avoid the manual errors during the operation of the machine.
- In fully computerized setup, the fully trained person or experienced person only will allow to work to avoid the treatment errors.
- Possible errors while operating the machines in teletherapy.
- Wrongly entering the treatment time or monitor unit for the treatment.
- Neglecting the warning signs displayed by the system will also lead to expectable errors.
- Routine monitoring the patient through CCTV is also very crucial one.

5. When we are setting the machine parameters (collimator angle, gantry angle, couch lateral movements) misplacing of these values lead to drastic errors in the treatment.
Possible errors in Brachytherapy:
- When compared to teletherapy, brachytherapy is less prone to an error that is also important to mind it.
- When inserting the catheters from the machine to patient, there is a chance placing in a wrong channel.
- In
computerized brachytherapy system radiation therapist may be do one error.
Suppose if two patients name is similar he/she should conform first verbally to
the patient. If, he/she fails to does that lead to severe impact on the
patient.
Overall the machine performance and its operation are in the hand of radiation therapist, because they are routinely working in that machine they are know very well others about the complications and errors in setups. So they should care those in mind to eradicate the incorrect treatment in radiotherapy
Questions:
1. What are the people required for successful run of the machine?
- Radiation Therapist
- Medical Physicist
- Dosimetrist
- All
is correct
Answer:
- All is correct
References:
- www.Dragon-tongue.com
- www.Variantruebeam.com
- Console controls
Treatment Machine Set-Up > Beam Modifiers
Treatment Administration > Patient Monitoring Systems
- Patient Monitoring Systems
- Direct visual
- Indirect Visual
- Two-way voice communication system
- Emergency situations
Patient Monitoring Systems (PMS) has been widely used in all radiotherapy centres. PMS brought to strict in regulations after faced a lot of discrepancies in the treatment. Different types of patient monitoring systems are in use.
They are listed below
- Direct visual system
- Indirect visual system
- Two-way voice communication system
The above mentioned systems are widely till
in use for monitoring the patients during the time of treatment. Because of the
movements and other issues during the treatment impose a bad impact on the
patient.
Direct visual System:
Direct visual is a one way of patient monitoring system. This system has been used in the olden days, at the time there is no advanced communication and other way of patient monitoring system. The direct visual system is useful in monitoring the patient during the radiation treatment.
Indirect visual system:
Indirect visual monitoring system is a type of patient monitoring system widely using till now in the radiotherapy. Time at which the radiation was started as treatment for cancer direct visual communication used widely (Lead window type). Later on the emergent of indirect visual patient monitoring systems slowly removed the usage of direct visual system by its unique advantage.
Two-way communication system:
Two-way voice communication system is that during the treatment it helps to communicate between the patient and Radiation Therapist. With the help of two way voice communication patient and Radiation therapist or Radiation therapist and patient can communicate at instant of treatment period.
- Patient Monitoring Systems
- Direct visual
- Indirect Visual
- Two-way voice communication system
- Emergency situations
Treatment Administration > Record and verify Systems
Treatment Administration > Portal Imaging
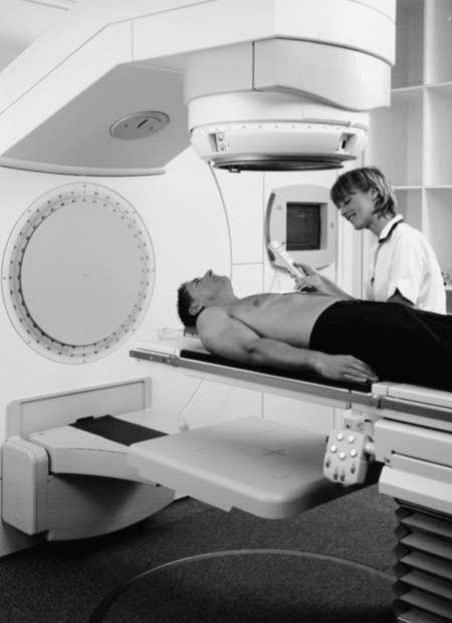
Portal imaging is the acquisition of images to conform the treatment
field setup before the execution of the concern treatment. Portal imaging will
be acquired with the help mega voltage beam. But, now a day this trend has been
modified by setting the x – ray tube in the gantry or changing the energy of
linear accelerator to ordinary KV imaging energy. In all the latest linear accelerator are
coming with Electronic Portal Imaging Device (EPID). In addition to that,
on-board imager (OBI) is attached with the machine to verify the treatment
field. But still EPID is in practice in all the linear accelerators.
Using portal imaging we can verify the treatment field is correct or not. But, it is not possible to get the good quality image to see the treatment field clearly. Because in diagnostic imaging photoelectric effect is predominant but, in therapy Compton Effect is more predominant than other effects. In Compton Effect the scattering of the photon beam would be there because of its high energy. Not only that but also Compton Effect doesn’t depend on atomic number of the material.
Above figure shows the EPID of Elekta machine.
Different types of portal imaging are,
1. Camera based Portal Imaging
2. Film based Portal Imaging
Camera based Portal Imaging:
In camera based portal imaging X-ray to light converter, mirror and camera would be used for portal imaging. The photon beam is allowed to fall on metal plate attached with phosphor and then fall on the slanted glass mirror, after that it will be catch by using the video camera.
Film based Portal Imaging:
Film based portal imaging is traditional medium of portal imaging. In Film based portal imaging the ready pack films or autoradiograph quality films are used for verification.
Advantages of Portal Imaging:
1. Treatment field verification during the treatment gives the quality treatment.
2. Images will be available immediately for reference.
3. While x-ray imaging patient have to be shift from treatment room to x-ray room it leads to unnecessary error in the setup.
Disadvantages of Portal Imaging:
1. Bulky attachment is one of the major disadvantages.
2. Poor image quality.
3. Not cost effective.
Questions:
1. Why image quality in portal imaging are very poor?
- Compton is predominant in therapy
- Because of high energy
- Photoelectric effect is dominant
- A and B is correct
- A and C is correct
- All
Answer:
- A and B is correct
References:
- The Physics of Radiation Therapy 4th Edition by Faiz. M. Khan
- www.pubmed.com
- www.BJR.com
- Portal imaging, K A LANGMACK, DPhil, Medical Physics Department,
Lincoln County Hospital, Greetwell Road, Lincoln, UK
Treatment Administration > Site Verification
Treatment Administration > Dose Verification
Dose verification system (DVS) is an important one to consider it. Due to the emergent of advanced technologies in radiotherapy machines and others more number of patients is getting radiation treatment. However, we don’t is it really they are getting the exact dose which is prescribed. Dose is the prime factor in determining the curative part of the treatment. It may lead to under and over dosage both cause the recurrence of cancer again. In radiotherapy only the successful rate of the treatment is considered only if, they survive more than five years.
For this purpose people introduced DVS to monitor the patient. The DVS can be done different methods by using different equipment. Only thing is that it shouldn’t alter the treatment outcome of the concerned persons.
The following systems is routinely using for DVS,
- Using Diodes, Dose Verification System.
- Film based, Dose Verification System.
- EPID based, Dose Verification System.
DVS using Diodes (MOSFET):
Dose Verification System consists of implantable MOSFET dosimeter for measuring radiation dosage at particular depths, an insertion tool to implant this dosimeter and reader system to receiving these doses. The reader has the ability to record the daily as well as the cumulative dosage. In DVS two Metallic oxide semiconductor field effect transistor (MOSFET) of measuring 2mm to 18mm which are permanently implanted into the patient body. The MOSFET will act as a radiation sensing part. Radiation doses can be monitored through wireless technology outside from the handheld controller. By using the software dose can be reviewed after the treatment. This device can also be used as reference marker in imaging.

Above figure shows the MOSFET dosimeter Setup
Film based DVS:
The film based Dose Verification System has been used till from the beginning of the DVS. Simply placing the radiographic film below the treatment site and expose with mega voltage beam of lesser to verify it. From the film the intensity can be read and dosage levels to be known by measuring with the help characteristic curve and densitometer.

EPID based DVS:
After the introduction
machines with EPID it becomes very easy to verify the patient treatment site
and sometimes dosage by special methods. The EPID based 3D dose verification
has to be done before the actual treatment of the patient. Detail work of 3D
dose verification done by Wouter van
Elmpt etal.
Questions:
1. Dose Verification System
increasing the,
- Accuracy of the treatment
- Quality of the treatment
- Survival indirectly by delivering the prescribed dose
- All
Answer:
- All
References:
- Dose Verification System—Radiation Detector for Radiation Therapy, a report by,Tina Marie Briere, PhD
- PhD thesis: “3D dose verification for advanced radiotherapy”, Wouter van Elmpt, PhD – Department of Radiation Oncology (MAASTRO), GROW – School for Oncology and Developmental Biology, Maastricht University Medical Centre, Maastricht, The Netherlands.
- National Horizon Scanning Centre, National Institute of Health Research, university of Birmingham
- The Dose Verification System (DVS) for cancer patients receiving radiation therapy, Scarantino CW, Beyer GP, Department of Radiation Oncology, Rex Cancer Center, 4420 Lake Boone Trail, Raleigh, NC 27607, USA.
- www.ncbi.nlm.nih.gov/pubmed
- www.waset.org
- The Physics of Radiation Therapy 4th edition by Faiz. M. Khan.
- www.medphys.org
- Journal of applied clinical medical physics.
- http://www.maestro-research.org/pageprincipale1.htm
Treatment Administration > Equipment Malfunctions
- Types
Documentation> Information in Treatment Record
- Tumor dose
- Energy and type of radiation
- Fraction
- Set-up instructions
Documentation > Elements of record Keeping
- Patient Identification
Documentation > Charge Capture Terminology
FREE Infographic What successful people believe. What successful people do
Dictionary of Cancer Terms
Need help understanding a word? Here is an electronic resource that gives meaning to Cancer terms and their usage.

StrengthsFinder 2.0